
Limb salvage surgery is a type of surgery primarily performed to remove bone and soft-tissue cancers occurring in limbs in order to avoid amputation. In recent years, limb salvage has been extended more and more to patients severely affected by chronic degenerative bone and joint diseases, such as rheumatoid arthritis, or those facing diabetic limb amputation or acute and chronic limb wounds.
As recently as 10 to 20 years ago, the surgical answer to aggressive tumors of the extremity was amputation. While this is necessary in certain cases today, many patients are treated with limb salvage, or limb sparing surgery, with similar results. These operations are designed to save the limb while removing the tumor. Special prostheses, bone grafts, and bone transplantation, are all techniques used in these surgeries.

After determining that limb salvage is appropriate for a particular patient, the doctor makes sure that the patient understands what the outcome of surgery is likely to be, that the implant may fail, and that additional surgeryeven amputationmay be necessary.
Physical and occupational therapists help prepare the patient for surgery by introducing the muscle-strengthening, ambulation (walking), and range of motion (ROM) exercises the patient will begin performing right after the operation.

During the five to 10 days the patient remains in the hospital following surgery, nurses monitor sensation and blood flow in the affected extremity and watch for signs that the patient may be developing pneumonia, pulmonary embolism, or deep-vein thrombosis.
The doctor prescribes broad-spectrum antibiotics for at least the first 48 hours after the operation and often prescribes medication (prophylactic anticoagulants) and antiembolism stockings to prevent blood clots. A drainage tube placed in the wound for the first 2448 hours prevents blood (hematoma) and fluid (seroma) from accumulating at the surgical site. As postoperative pain becomes less intense, mild narcotics or anti-inflammatory medications replace the epidural catheter or patient-controlled analgesic pump used to relieve pain immediately after the operation.

Our hospitals are located in the northern part of the country specially in the NCR region within a distance of 20-50 kms from the New Delhi airport. Our hospitals are super specialty in the fields of Neurosurgery, Cardiology, Joint Replacement, Cancer Care, Liver and Kidney Transplants and many other brances of medicine. Some of our hospitals specialize only in Joint Replacements and Arthroscopies.
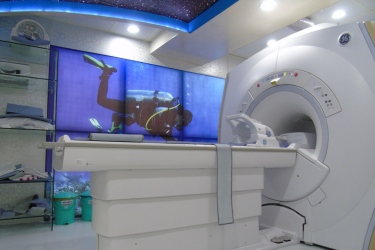
We have the latest MRI, CT Scan, Digital X-Ray, Bone Densitometry (DEXA), Mammography, Ultrasound, Colour Doppler which gives us the diagnostic confidence for providing the right treatment.
Modular fully equipped Operation Theatres with Computer Navigation and C-Arm backed by a state of art ICU helps us in providing world class treatment to our patients.

Our doctors include some of the most famous names in the world of medicine when it comes to Joint Replacements and Arthroscopies. Dr. Mukesh Jain, Dr Ashok Rajgopal, Dr. J. Maheshwari, Dr Subhash Jangid, Dr Praveen Tittal, Dr Anubhav Jain are some of the names which command respect all over the world for the kind of work done by them in their lifetime.
Kim Brian from the Sacramento County of California, USA came to India to get Hip Replacement Surgery done. He travelled alone because he could not afford the expenses for an attendant. His surgery was done by Dr IPS Oberoi at Artemis Health Institute. Watch this video where Kim is sharing his experiences.
Mr. Mark Wisman suffered an injury to his knee while driving his pickup. For years he lived in pain and finally landed in India for Total Knee Replacement Surgery to be done by Dr. Ashok Rajgopal at Medanta Medicity. He had some interesting things to say about treatment in India specially the cost of the treatment.
Mr Mphoso got spine surgery done in Pretoria, South Africa in Dec 2016 but did not get relief from back pain. His search ended with Dr Vikas Khaturia in India who performed Revision Spine Surgery at one level and Fusion Surgery at another Level. The surgery was done in July 2017 and the delighted patient has this to say.